FOR YOUR HEALTH: Blood Donors Power Stroke Survivor’s Medical Dream
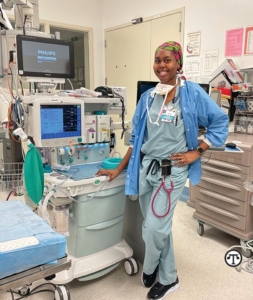 (NAPSI)—What seemed like an ordinary morning for four-year-old Kelly Bernard Igwe became life-altering. She woke up with her left arm completely numb, as if she had slept on it wrong. But this was not the temporary tingling that comes from an awkward sleeping position.
(NAPSI)—What seemed like an ordinary morning for four-year-old Kelly Bernard Igwe became life-altering. She woke up with her left arm completely numb, as if she had slept on it wrong. But this was not the temporary tingling that comes from an awkward sleeping position.
Her mother noticed something was different. Bernard Igwe was pulling up her clothing with only one arm, and she developed what her mother initially thought was an adorable, crooked smile. When Bernard Igwe began walking with a limp that persisted for days, her mother knew something was seriously wrong. The diagnosis revealed that Bernard Igwe, who was born with sickle cell disease, had suffered a stroke.
A Silent Crisis
Around 10 percent of children with sickle cell disease – the most common inherited blood disorder in the U.S. – experience a symptomatic stroke, with the risk being highest between ages two and five. Without preventative treatments such as regular blood transfusions, at least 60 percent of these children are at risk for another stroke.
What followed for Bernard Igwe was a regimen of blood transfusions every four to six weeks throughout her childhood—a medical lifeline that continues today through seven to eight units of red blood cell exchanges, a non-surgical therapy that removes abnormal red blood cells and replaces them with healthy ones from blood donors every six to seven weeks.
“I wouldn’t be alive without transfusions,” Bernard Igwe said. “There was a high likelihood of me having another stroke had I not started getting blood transfusions when I was young.”
Bernard Igwe’s journey highlights the devastating impact of sickle cell disease and the transformative power of blood donations. Sickle cell disease distorts soft, round red blood cells into hard, crescent shapes that block blood flow and oxygen delivery, causing severe pain, organ damage, and life-threatening complications such as strokes.
Joined by Blood
Frequent blood transfusions can make finding compatible blood more difficult when patients with sickle cell disease develop antibodies. Blood donors who are Black are almost three times more likely to be a match for these patients compared to other donors—making the increase in African American donors critical.
To help ensure these lifesaving treatments remain available, the American Red Cross is mobilizing communities through its fall Joined by Blood activation, hosting more than 750 blood drives nationwide through partnerships with the Sickle Cell Disease Association of America, historically Black colleges and universities, Black Greek organizations, Delta Air Lines and more.
Empowered to Dream
Rather than limiting her aspirations, the transfusions became Bernard Igwe’s launching pad. Throughout childhood, she excelled as a student and athlete, then pursued a career in healthcare after being inspired by her own medical providers. Today, she works as a Certified Registered Nurse Anesthetist, transforming her personal resilience into hope for others.
“Earning my doctorate and becoming a CRNA was a lifelong dream,” Bernard Igwe said. “Persevering through school despite my health challenges is something I’m really proud of.”
Bernard Igwe’s story shows how blood donations don’t just sustain life—they fuel dreams and careers.
“It is so important to donate blood if you’re able,” Bernard Igwe said. “Many of us rely on blood donations to live.”
How You Can Help
The Joined by Blood activation creates a powerful connection between donors and patients, giving those with sickle cell disease the security of knowing their communities stand ready to support them, while empowering donors to tap into their lifesaving power. To help people living with sickle cell disease, schedule an appointment to give blood by visiting RedCrossBlood.org/OurBlood or calling 1-800-RED-CROSS (1-800-733-2767).


 Winter is coming, so it’s a good idea to get your snow blower ready now to clear your way.
Winter is coming, so it’s a good idea to get your snow blower ready now to clear your way.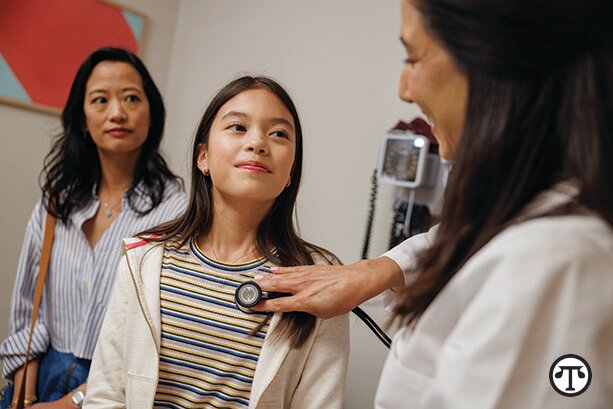 For a happier holiday season, remember to take care of your health.
For a happier holiday season, remember to take care of your health.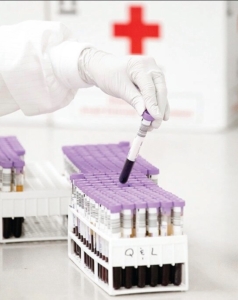
 Now is the time to fight the flu. Fortunately, it can be fast and easy to get a flu shot.
Now is the time to fight the flu. Fortunately, it can be fast and easy to get a flu shot.
 Depending on your age and health status, vaccines for flu, COVID-19, RSV, and pneumococcal disease may be recommended for you.
Depending on your age and health status, vaccines for flu, COVID-19, RSV, and pneumococcal disease may be recommended for you.
 (NAPSI) – Have you or someone you love been diagnosed with Alzheimer’s disease? Alzheimer’s is a brain disease that affects memory, thinking and behavior. It’s the most common cause of dementia, which is a word used to describe memory loss and other thinking problems that affect daily life. (Source: Alzheimer’s Association)
(NAPSI) – Have you or someone you love been diagnosed with Alzheimer’s disease? Alzheimer’s is a brain disease that affects memory, thinking and behavior. It’s the most common cause of dementia, which is a word used to describe memory loss and other thinking problems that affect daily life. (Source: Alzheimer’s Association) Taking small steps now can protect your health today and into the future.
Taking small steps now can protect your health today and into the future.